A latest cyberattack on the College of Mississippi Medical Heart shut down clinic operations for 9 days, disrupting appointments and entry to care throughout Mississippi. In response to the middle’s personal official system replace, scheduling, communications, and medical workflows had been all impacted.
9 days with out regular entry to care is not only a cybersecurity downside. It’s a market construction downside.
The College of Mississippi Medical Heart is just not merely one other hospital. It’s Mississippi’s solely tutorial medical heart and serves because the state’s main hub for specialty care, doctor coaching, and sophisticated companies. By its personal description, it supplies ranges of care “unavailable wherever else within the state.” That focus means when UMMC goes down, a lot of Mississippi’s superior care capability goes down with it.
In a aggressive system, that ought to not occur.
When a serious supplier in most industries goes offline, others step in. Capability shifts. Prospects reroute. The system bends however doesn’t break. In Mississippi, it broke.
A System Constructed to Focus
That fragility is just not an accident. It’s the results of coverage.
Mississippi has lengthy enforced certificate-of-need legal guidelines that require authorities approval earlier than new hospitals, surgical facilities, or main medical companies can open or broaden. These legal guidelines are sometimes justified as cost-control measures. In observe, they restrict entry and shield incumbents.
Mississippi’s model is among the many extra restrictive. Functions can price tens of hundreds of {dollars}, and current suppliers are allowed to problem potential rivals. The impact is predictable. Fewer entrants. Slower growth. Much less redundancy.
Coverage evaluation by the Mississippi Heart for Public Coverage discovered that, with out CON restrictions, Mississippi might have supported 30 p.c extra rural hospitals and 13 p.c extra ambulatory surgical facilities, thereby growing entry in underserved areas. A comparable state with out such restrictions would have roughly 165 hospitals, in contrast with Mississippi’s 116, a distinction of greater than 30 p.c in complete capability in 2017.
That lacking capability issues most when one thing goes improper.
Fragility Has Penalties
The cyberattack didn’t create Mississippi’s entry downside. It uncovered it.
When a single establishment serves because the spine of a state’s healthcare system, any disruption turns into systemic. Sufferers don’t merely go elsewhere. In lots of circumstances, there may be nowhere else to go.
Meaning delayed diagnoses, postponed remedies, and worsening circumstances. It means longer wait occasions in an already strained system. And in excessive circumstances, it will probably imply preventable hurt.
Throughout the nation, wait occasions for doctor appointments are already rising, notably for main and specialty care. Programs with restricted competitors are much less capable of take in shocks, making these delays much more extreme when disruptions happen.
That is what lack of competitors appears to be like like in observe. Not simply larger costs, however lowered resilience.
The Financing Downside
Market construction is simply a part of the story. The way in which healthcare is financed amplifies the issue.
Most healthcare {dollars} don’t circulation via sufferers. They circulation via insurers, employers, and authorities packages. That disconnect weakens crucial sign in any market: worth.
When sufferers will not be paying out of pocket, suppliers compete much less on worth and extra on navigating reimbursement techniques. Administrative prices rise. Innovation slows. Capability turns into inflexible relatively than responsive.
That is the core situation recognized within the Empower Sufferers framework. Healthcare in america is dominated by third-party management relatively than affected person decision-making.
The result’s a system that’s each costly and fragile.
What Competitors Appears to be like Like
When competitors is allowed, the outcomes differ.
Clear suppliers such because the Surgical procedure Heart of Oklahoma publish costs upfront and infrequently ship care at considerably decrease price than conventional hospital techniques. Direct Main Care practices supply quicker entry, longer visits, and predictable pricing by working outdoors insurance coverage billing.
These fashions do greater than cut back prices. They add capability. They create options. They make the system extra resilient.
If one supplier goes offline, others can be found.
Mississippi has fewer options as a result of coverage has restricted their development. Even when regulators accredited a brand new hospital in Biloxi, the method revealed how tough it’s so as to add capability. The state issued a certificates of want in 2012 for a substitute facility, however incumbent hospitals sued to dam the mission, delaying it for years, arguing it was not a real substitute. That extended battle stemmed from the unique plan to construct a brand new hospital to interchange Gulf Coast Medical Heart after it was destroyed by Hurricane Katrina. Briefly, even apparent neighborhood wants will be slowed by authorized challenges from current suppliers.
The sample continues: latest consolidation has additional strengthened dominant techniques on the Gulf Coast, and policymakers pursue solely incremental adjustments to certificate-of-need legal guidelines, whereas others name for a broader overhaul of the state’s restrictions.
A Warning for Policymakers
The Mississippi cyberattack needs to be considered as a warning, not an anomaly. It revealed how weak a healthcare system turns into when competitors is restricted and capability is concentrated. What appears to be like environment friendly on paper will be fragile in observe.
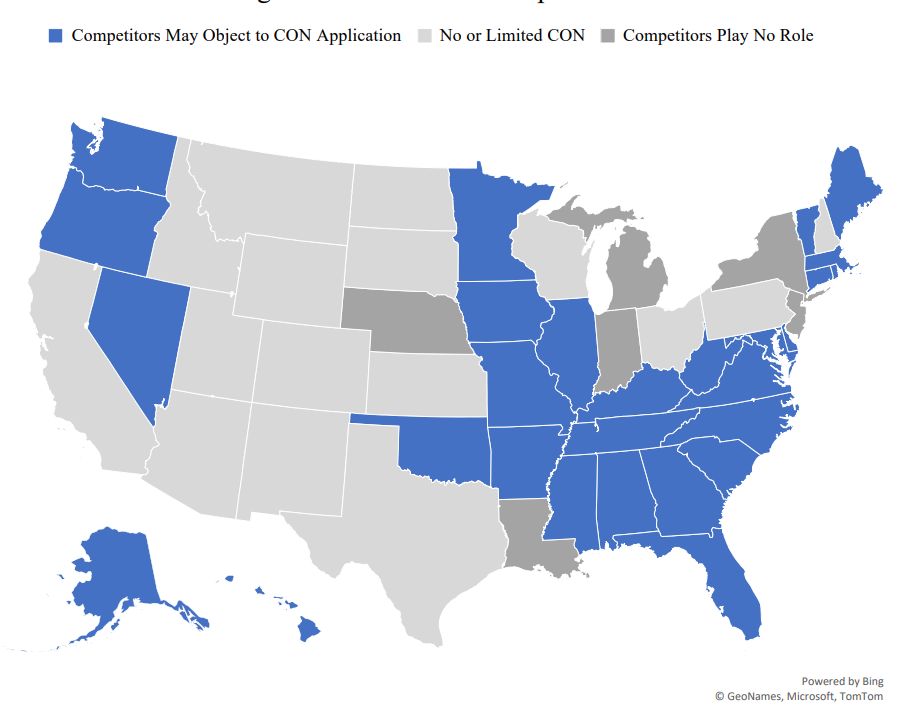
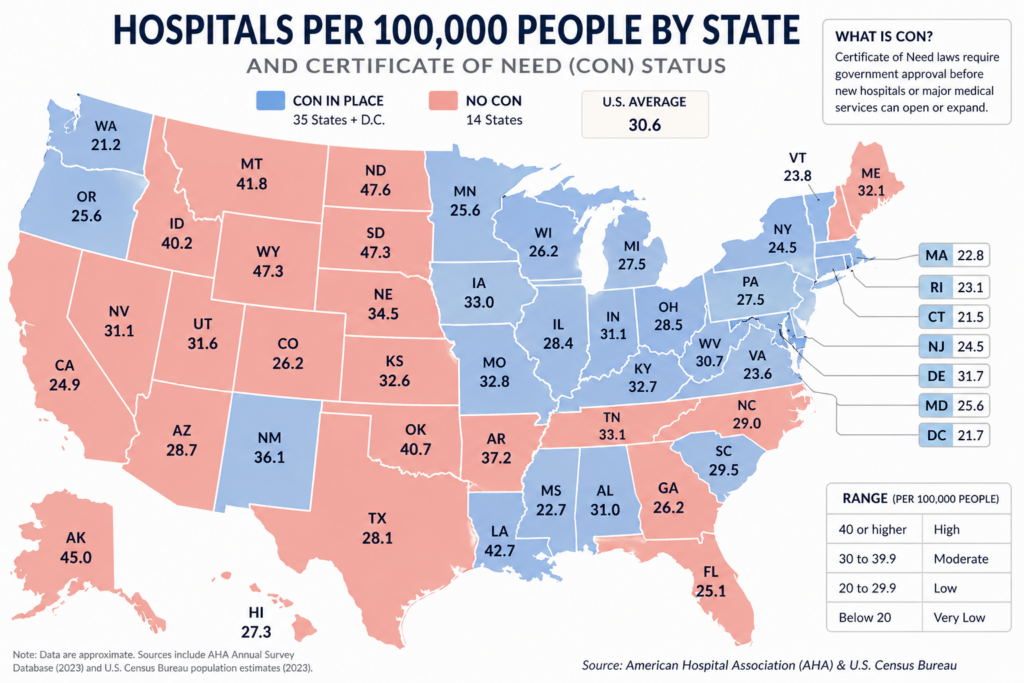
Mississippi is just not an outlier. 35 states and DC function underneath certificate-of-need legal guidelines that restrict the variety of new suppliers and growth. States have been working to enhance their CON legal guidelines, reflecting a rising recognition that the present construction is just too inflexible. However incremental reform won’t remedy a structural downside.
A Higher Path Ahead
A extra resilient healthcare system that empowers sufferers requires greater than cybersecurity upgrades. It requires coverage change.
First, take away limitations to entry that stop new suppliers from coming into the market. In Mississippi, the state might assist 30 p.c extra rural hospitals and 13 p.c extra ambulatory surgical facilities, that means extra choices for sufferers and extra capability when disruptions happen.
Second, shift financing towards affected person management. When people handle their very own healthcare {dollars}, they’ve an incentive to hunt worth, examine choices, and demand higher service.
Third, cut back regulatory burdens that divert assets from care to compliance.
These adjustments wouldn’t solely decrease prices. They’d make the system stronger.
The Actual Lesson
Mississippi’s healthcare system didn’t fail due to a cyberattack alone. It failed as a result of it lacked the flexibleness and redundancy to reply. One hospital system ought to by no means be a single level of failure for a whole state.
The way in which to forestall that isn’t extra centralization. It’s extra competitors, extra capability, and extra affected person management. That’s the lesson Mississippi gives — and it’s one policymakers throughout the nation ought to take critically.

